The normal infranodal conduction system divides into the right and left bundles, the latter is further subdivided into anterior and posterior divisions or “fascicles.” Disruption of both fascicles produces the familiar left bundle branch block (LBBB) pattern, but each fascicle can be affected independently – resulting in either left anterior fascicular block (LAFB) or left posterior fascicular block (LPFB). When the left anterior fascicle is disrupted, current passes along the posterior fascicle and the left ventricle is depolarized in a leftward/upward direction – producing left axis deviation (and often an extreme left axis deviation, i.e., more than 45 degrees of leftward deviation). Criteria for diagnosing LAFB include:
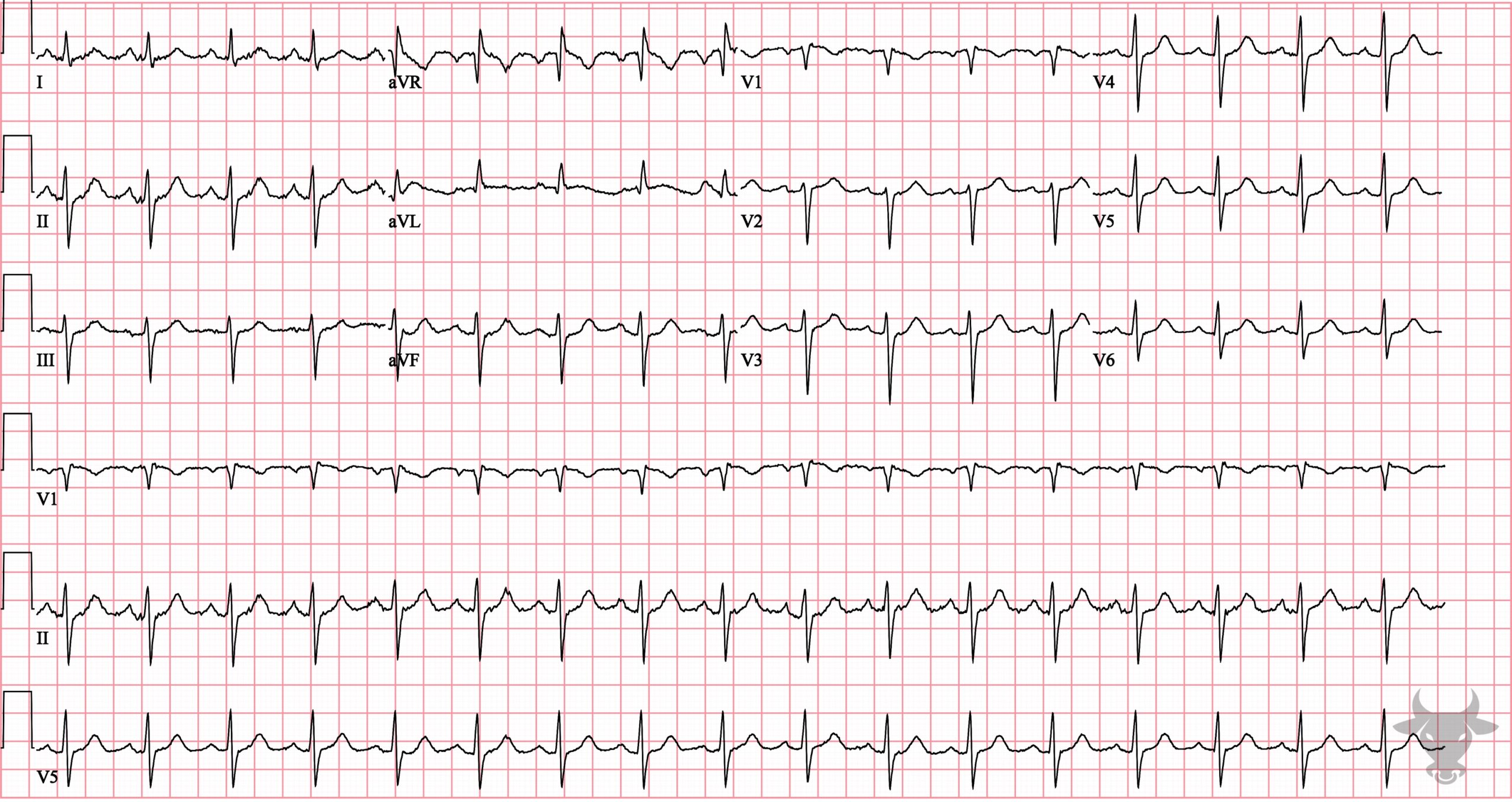
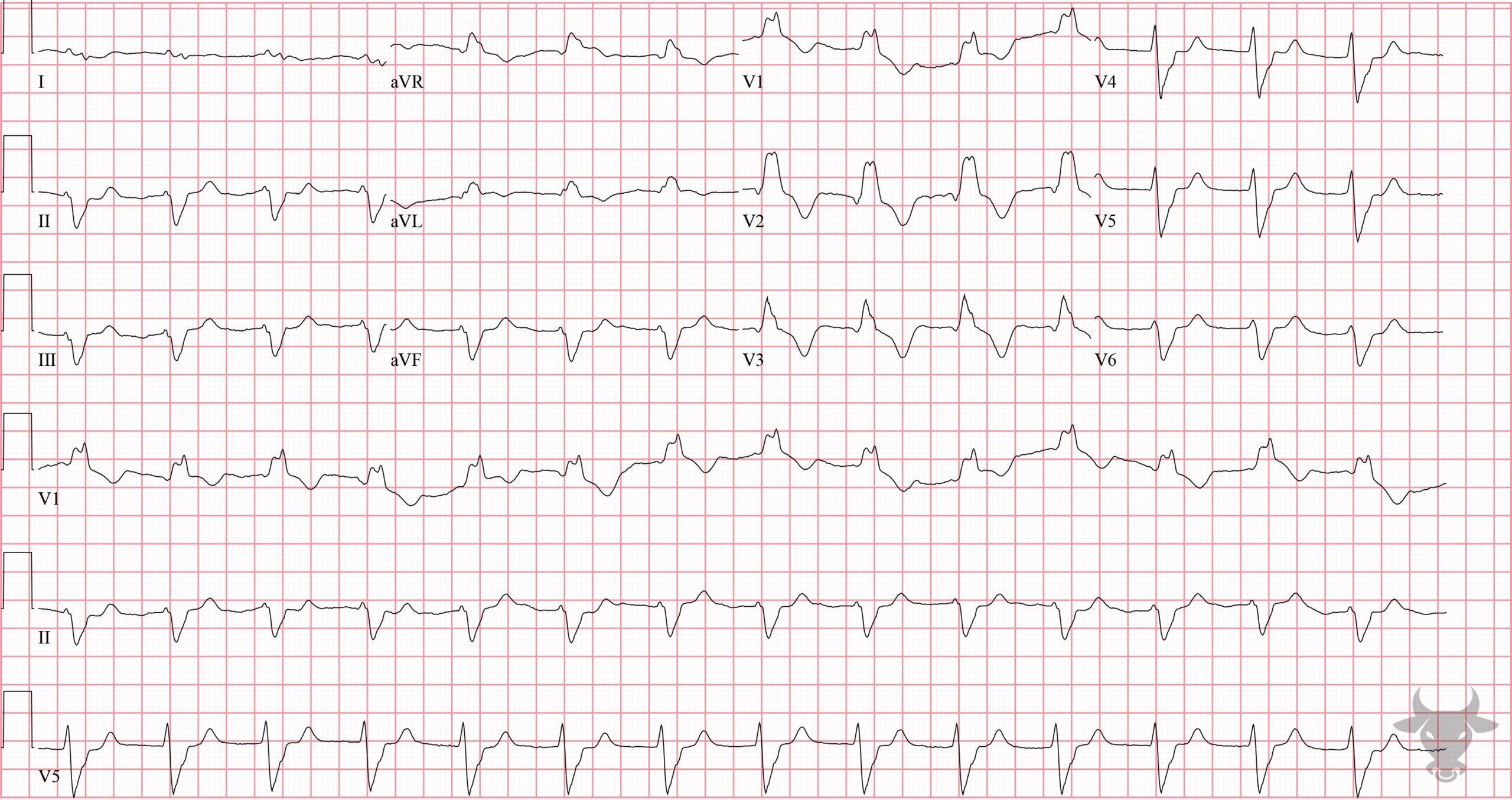
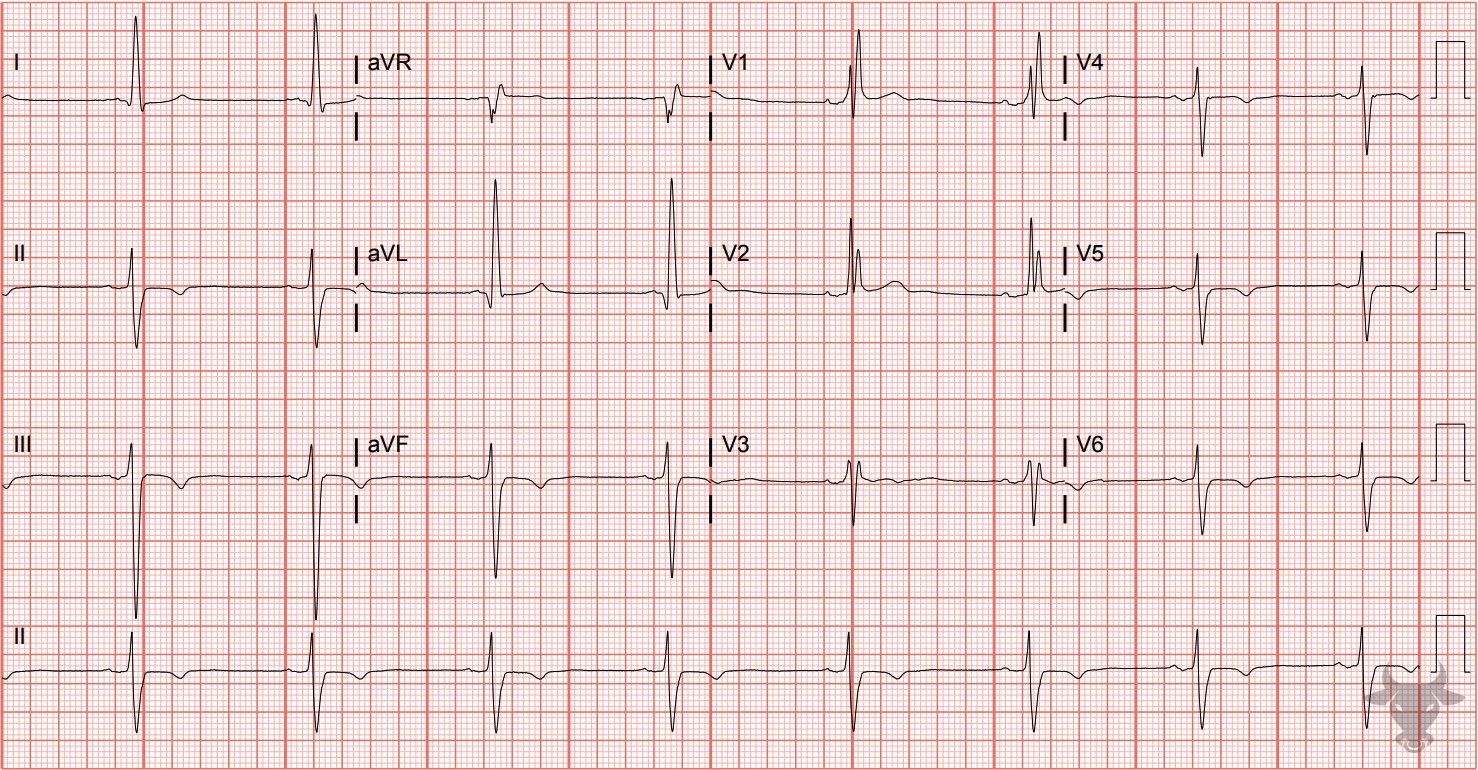
- Left axis deviation (usually > 45 deg)
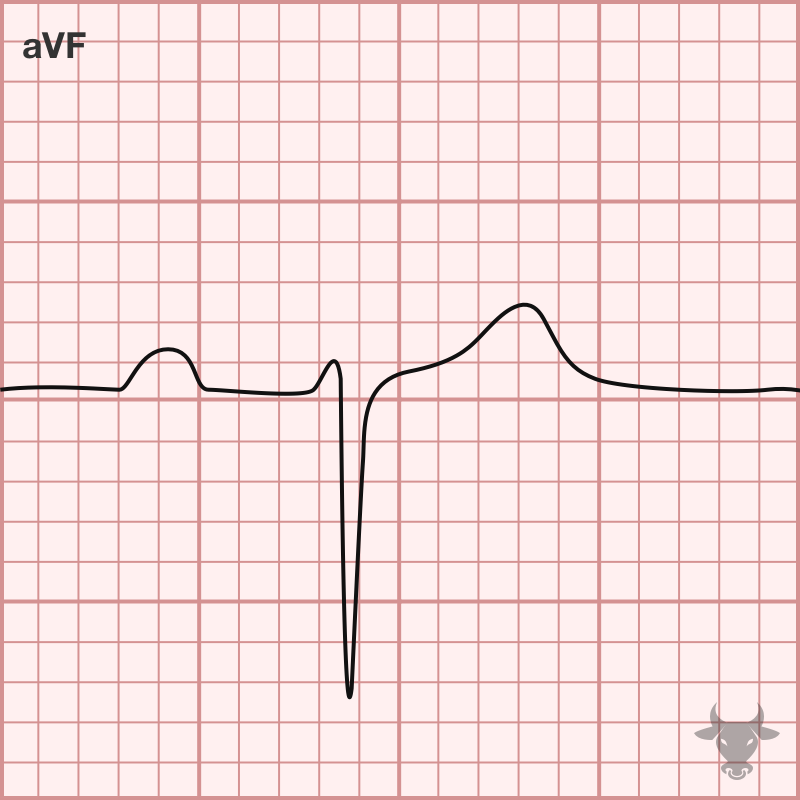
- Small q waves with large R waves (“qR complexes”) in I and aVL
- Small r waves with large S waves (“rS complexes”) in II, III, and aVF
- Normal or slightly prolonged QRS duration (80-110 ms)
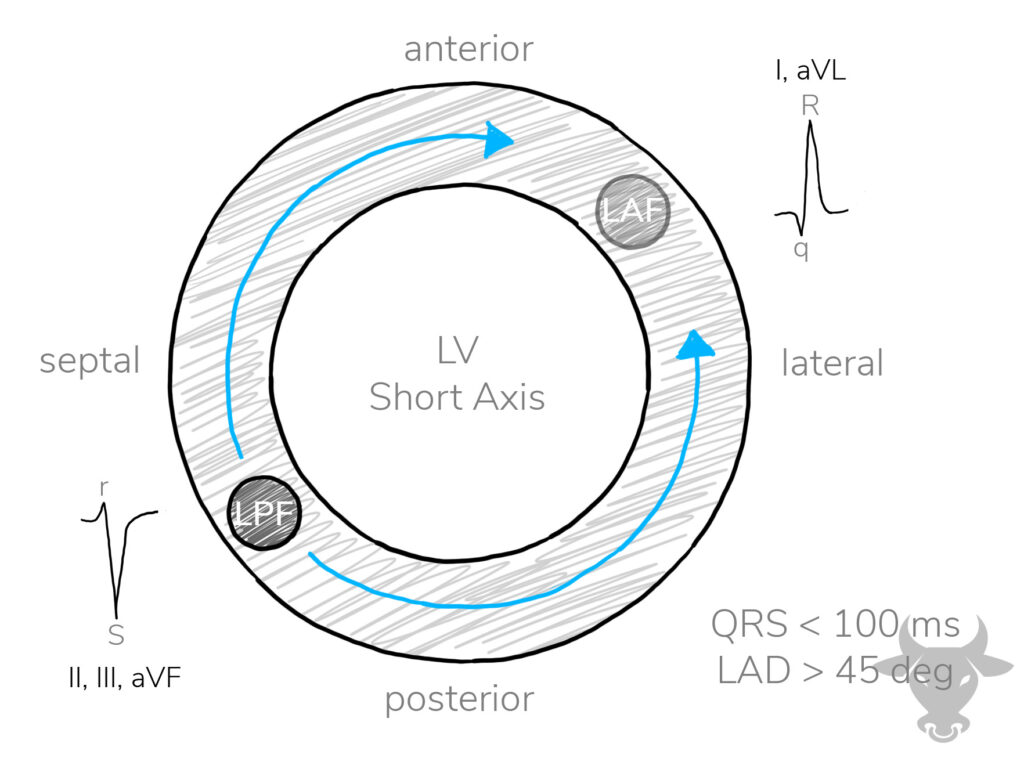
Locations of the anterior and posterior fascicles within the left ventricle. The curved blue arrows demonstrate the direction of depolarization when the left posterior fascicle fails, leading to left axis deviation. LV, left ventricle; LPF, left posterior fascicle; LAF, left anterior fascicle; LAD, left axis deviation.